Major depressive disorder

Definition
Major depressive disorder (MDD) is a condition characterized by a long-lasting depressed mood or marked loss of interest or pleasure (anhedonia) in all or nearly all activities. Children and adolescents with MDD may be irritable instead of sad. These symptoms, along with others described below, must be sufficiently severe to interfere significantly with the patient's daily functioning in order for a person to be diagnosed with MDD.
Description
Major depressive disorder is a serious mental disorder that profoundly affects an individual's quality of life. Unlike normal bereavement or an occasional episode of "the blues," MDD causes a lengthy period of gloom and hopelessness, and may rob the sufferer of the ability to take pleasure in activities or relationships that were previously enjoyable. In some cases, depressive episodes seem to be triggered by an obviously painful event, but MDD may also develop without a specific stressor. Research indicates that an initial episode of depression is likely to be a response to a specific stimulus, but later episodes are progressively more likely to start without a triggering event. A person suffering major depression finds jobrelated responsibilities and such other tasks as parenting burdensome and carried out only with great effort. Mental efficiency and memory are affected, causing even simple tasks to be tiring and irritating. Sexual interest dwindles; many people with MDD become withdrawn and avoid any type of social activity. Even the ability to enjoy a good meal or a sound night's sleep is frequently lost; many depressed people report a chronic sense of malaise (general discomfort or unease). For some, the pain and suffering accompanying MDD becomes so unendurable that suicide is viewed as the only option; MDD has the highest mortality rate of any mental disorder.
Major depressive disorder may be limited to a single episode of depression; more commonly, it may become a chronic condition with many episodes of depressed mood. Other symptoms that may develop include psychotic symptoms (bizarre thoughts, including delusional beliefs and hallucinations ); catatonia ; postpartum onset (sometimes accompanied by psychotic symptoms); and seasonal affective disorder , or SAD.
Such conditions as postpartum depression and seasonal affective disorder accompany MDD only under certain circumstances. Postpartum depression begins within four weeks of giving birth. Women with this disorder experience labile mood (frequent drastic mood changes). They may feel helpless and unable to care adequately for their infant, or they may be completely uninterested in the child. The symptoms of postpartum depression are much more severe than those of the relatively common "new baby blues," which affect up to 70% of new mothers. The presence of psychotic symptoms in the mother, too many ruminations (obsessive thoughts), or delusions about the infant are associated with a heightened risk of serious harm to the child. The symptoms of postpartum depression are usually attributed to fluctuations in the woman's hormone levels and the emotional impact of bearing a child. The condition is especially likely to occur in women who were highly anxious during pregnancy or had a previous history of mood disorder. Seasonal affective disorder (SAD) is also more common in women than in men; in this case, symptoms of MDD typically begin in fall and winter, especially in northern latitudes in the United States and Canada. Exposure to natural light is limited during the winter in these areas, but the symptoms of SAD typically improve during the spring and summer.
Causes and symptoms
Causes
Because MDD is a relatively common mental disorder, researchers have performed a range of different studies to identify possible underlying causes. Three types of causes are commonly identified: intrapsychic, environmental, and biological.
INTRAPSYCHIC. Since Sigmund Freud attributed the development of mental disorders to intrapsychic (occurring inside the mind) conflicts occurring during early childhood, a sizeable number of theorists have suggested that MDD results from a tendency to internalize negative events. Cognitive behavioral treatment models assume that a person's interpretation of situations is responsible for the development of depression rather than the events themselves. Some people blame themselves for negative experiences while attributing positive outcomes to external sources; they may tend to feel guilty, undeserving, and eventually depressed. For example, they may think of their present job as something they obtained by a chance stroke of good luck; at the same time, they may regard being laid off as something they brought on themselves. When these patterns of thought become habitual, they lead to a style of coping characterized by a view of oneself as worthless, ineffectual, and inferior. In some cases, people pick up these patterns of thinking from their parents or other family members.
Another theory regarding intrapsychic causes attributes depression to so-called "learned helplessness." This theory grew out of research studies on animal learning, comparing dogs that were able to escape from mild electric shocks to dogs that could not escape. The researchers discovered that the dogs who could not escape the mild shocks became passive; later, when they were put in a situation in which they could escape the shocks, they made no attempt to do so but simply lay on their stomachs and whimpered. The animals had, in short, learned to be helpless; they had learned during the first part of the experiment that nothing they had done had any effect on the shocks. Applied to human beings, this theory holds that people tend to become depressed when they have had long-term experiences of helplessness— as would be the case for abused children. Later, when the children have become adults, they do not see themselves as grownups with some control over their lives; they continue to react to setbacks or losses with the same feelings of helplessness that they had as children, and they become depressed.
ENVIRONMENTAL. Environmental theories of the etiology (causation) of MDD emphasize the role of external events in triggering depression. According to this perspective, people become depressed primarily due to unfortunate circumstances that are difficult to change. In some cases, these misfortunes may include environmental disasters or personal losses; but such other factors as low socioeconomic status, oppression associated with one's sex or race, or unpleasant or frustrating relationships are also thought to contribute to depression.
BIOLOGICAL. Ancient medicine alleged that one's state of mind was related to the presence of specific "humors," or fluids, in the body, and various theories have emerged since the eighteenth century regarding possible constitutional factors in humans that affect mood. In recent years, researchers have found numerous abnormalities in the neuroendocrine systems, neurotransmitters , and neuroanatomy of the brains of both children and adults with MDD, as well as strong evidence for genetic factors in MDD.
Levels of cortisol, a hormone associated with the human "fight-or-flight" response, have long been studied as possible biological markers for depression. In many adults, cortisol levels rise when the person is acutely depressed and return to normal when the depression passes. Research findings have been inconsistent regarding cortisol levels in children and adolescents, although there is some evidence that higher levels of cortisol secretion are associated with more severe depressive symptoms and with a higher likelihood of recurrence. As of 2002, however, cortisol levels are not considered to be reliable enough to be useful in diagnosing MDD.
Another biological factor that has been studied in humans are changes in the levels of neurotransmitters, which are chemicals that conduct nerve impulses across the tiny gaps between nerve cells. Variations in the levels of certain neurotransmitters have been researched for many years due to their importance in the brain's limbic system, which is the center of emotions and has many important pathways to other parts of the brain . In depression, the system that regulates a neurotransmitter called serotonin does not function properly. A group of medications known as serotonin specific reuptake inhibitors, or SSRIs, are assumed to be effective in relieving depression because they prevent serotonin from being taken back up too quickly by receptors in the brain.
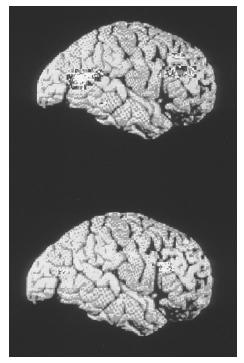
Differences in the anatomical structure of the brains of children and adults with MDD have suggested several possible explanations for its development. In particular, the prefrontal cortex has been thought to play a role, on the basis of findings in stroke patients with damage to the prefrontal area of the brain, and in children and adults with MDD. Researchers found that stroke patients experienced more severe depression if their stroke occurred closer to the frontal lobe of the brain; similarly, people with MDD have been found to have decreased frontal lobe volume. Studies of depressed children and adults included subjects who were currently depressed as well as those with a history of depression who were in remission, which suggests that abnormalities in the frontal lobe may be a structural marker of depression. Other neurological studies have reported lower levels of electrical activity in the left frontal cortex among depressed subjects (including the infants of depressed mothers) compared to persons who are not depressed.
Researchers have also been interested in the relationship of genetic factors to depression. It has been known for many years that depression tends to run in families. Convincing evidence of the heritability of depression has been obtained by comparing identical twins (who have identical genetic inheritances) with fraternal twins; these studies have consistently found a higher likelihood of depression between identical than between fraternal twins. Other data indicate that people with a higher genetic risk of depression are more likely to become depressed following a stressful event than people with fewer genetic risk factors.
Symptoms
The core symptom of major depression is a sad mood that does not go away. While most people have occasional days when they feel out of sorts, persons with MDD experience low feelings that build gradually over a period of days or weeks. They are usually not able to "snap out of it" even when something positive happens. In some cases, the symptoms are preceded by an obvious loss or painful event, such as divorce or a death in the family, but the disorder may also appear to begin "out of the blue." People with MDD often appear sad, irritable, and easily moved to tears. They may sleep poorly and complain of vague physical aches and pains; experience sexual difficulties or loss of interest in sex; drop out of social activities; and come across to others as unhappy or lacking in energy. Some people with MDD may deny that they feel depressed, but they lose their enthusiasm for hobbies or work they once found enjoyable and rewarding. Children and adolescents present with many of these same characteristics, but they may often appear easily frustrated and cranky instead of sad. The symptoms of MDD can be summarized as follows:
- Disturbed mood (sad, hopeless, discouraged, "down in the dumps") during most of the day.
- Loss of interest or pleasure in activities.
- Change in appetite nearly every day, leading either to weight gain or to loss of 5% of body weight. In children, this symptom may appear as a failure to make normal weight gains related to growth.
- Insomnia (waking in the middle of the night and having difficulty returning to sleep, or waking too early in the morning) or hypersomnia (sleeping much more than normal).
- Psychomotor retardation (slowed thinking, speech, body movements) or agitation (inability to sit still, hand-wringing, pulling at clothing, skin, or other objects) that is apparent to others.
- Sense of worthlessness or unreasonable guilt over minor failings.
- Problems with clear thinking, concentration, and decision-making.
- Recurrent thoughts of death or suicide, or making a suicide attempt.
Demographics
Recent research indicates that 4.9% of the population of the United States meets the diagnostic criteria for MDD at any given time, but 17.1% will experience at least one episode of the disorder at some point during their lives. While the disorder may affect people at any age, it is most commonly diagnosed in young adults in their twenties. For reasons that are not well understood, women are twice as likely to develop MDD as are men; prior to puberty, however, MDD is about equally common in girls and boys. Adolescence is a high-risk period for MDD; while suicide may result from impulsive behavior under stress rather than from MDD, it is noteworthy that about 14% of all teenage deaths are due to suicide. The figures for gay and lesbian youth indicate that as many as 20%–35% make suicide attempts. Other risk factors include Hispanic ethnicity; younger age at onset; lower levels of education or income; and being separated or divorced.
Depression appears to have become a more common disorder over the past century. Epidemiologists studying the incidence of depression across time compared groups of people born between 1917 and 1936, between 1937 and 1952, and between 1953 and 1966; their results indicated that the rate of depression increased progressively from one generation to the next. While no single explanation for the rise in depressive disorders emerged, some researchers have suggested that the breakdown of social support networks caused by higher rates of family disruption and greater social mobility may be important contributing factors.
Diagnosis
Major depressive disorder may be diagnosed when a person visits his or her family doctor with concerns about mood, changes in appetite or sleeping patterns, and similar symptoms. Doctors in family practice, in fact, are more likely to be consulted by patients with depression than doctors in any other medical specialty. In addition, a large proportion of people discuss depressed feelings with their clergyperson, who, in the mainstream Christian and Jewish bodies, has typically been trained to recognize the signs of depression and to encourage the person to see their doctor. In some cases the patient may be brought to see the doctor by a concerned spouse or other family member.
The diagnosis of MDD involves a constellation of symptoms in addition to depressed mood. After taking a careful history, including asking the patient about his or her sleeping patterns, appetite, sex drive, and mood, the doctor will give the patient a physical examination to rule out other possible causes of the symptoms. Certain other disorders may resemble MDD, including cognitive dysfunction caused by the direct effects of a substance (drug of abuse, medication, or toxic chemical); various medical conditions (i.e., an underactive thyroid gland; strokes; or early stages of dementia ), or other mental disorders. Such stressful life events as normal bereavement may also produce behaviors similar to those associated with MDD; while a bereaved person may appear to have many of the characteristics of MDD, the disorder would not be diagnosed unless the symptoms continued for more than two months or were extreme in some way. As part of the diagnostic interview, the doctor may give the patient a brief screening questionnaire, such as the Beck Depression Inventory , in order to obtain a clearer picture of the symptoms. In addition to interviewing the patient, the doctor may talk to family members or others who can provide information that the patient may forget, deny, or consider unimportant.
The diagnosis of MDD is complicated by the fact that people with MDD frequently suffer from other mental illnesses at the same time, including anxiety disorders, substance abuse problems, and personality disorders . Given that the patient's symptoms may vary according to age, sex, and stage of the illness, some clinicians have suggested that MDD may actually be a collection or group of disorders with a small number of underlying core symptoms rather than a single entity.
The diagnosis of a person with MDD may also include certain specifiers, including the severity and chronicity of the disorder; the presence of psychotic features (delusions or hallucinations) or catatonia (remaining motionless for long periods of time, and other peculiarities of posture, movement, or speech); melancholia (depressed mood that is worse in the morning; early morning wakening; psychomotor retardation or agitation; significant weight loss; or inappropriate guilt); and information regarding postpartum status. If the depression is currently in remission, this fact is also commonly listed as a diagnostic specifier.
Treatments
Because MDD can have a devastating impact on a person'slife, the importance of effective treatment cannot be overestimated. Treatment strategies have evolved over
Psychotherapy
Cognitive psychotherapies for depression are based on the belief that depressed people perceive themselves and the world in unrealistically negative ways. Considerable research has been done regarding the cognitive dimension of depression; for example, studies find that depressed people pay more attention to negative events than to positive ones, and that dwelling on unpleasant experiences prolongs and worsens depressive episodes. Cognitive therapists help patients identify the automatic thoughts that lead them to anticipate poor outcomes or to interpret neutral events in negative ways. The patient is also encouraged to challenge negative thoughts by comparing his or her expectations of events with actual outcomes.
Evidence that poor interpersonal relationships may heighten vulnerability to depression, along with findings that depressed adults and depressed children tend to provoke negative reactions from other people, has prompted the use of social skills training as a form of treatment. In this type of therapy, patients are trained to recognize actions and attitudes that annoy or distance other people, and to replace these behaviors with more appropriate ones. Social skills training may be particularly helpful to depressed persons who tend to isolate themselves and have lost confidence in their ability to develop healthy relationships. This treatment model promotes the idea that depression is likely to lift when the patient becomes adept at making new friends and establishing rewarding social supports.
Psychodynamic psychotherapy is often effective in treating patients with MDD whose depression is related to unresolved issues from the past, particularly abuse or other painful childhood experiences. The growth of insight into one's emotional patterns, as well as the supportive aspects of this form of therapy, offers considerable relief from emotional pain to many patients.
Medications
The use of medications in the treatment of depression began in the late 1950s with the successful introduction of tricyclic antidepressants and MAO inhibitors. Treatment of depression with medications has greatly increased since the advent of selective serotonin reuptake inhibitors (SSRIs) such as fluoxetine (Prozac) and sertraline (Zoloft). While these medications are no more effective than their predecessors, they have fewer side effects and are much safer for patients who may be likely to overdose. Selecting the optimal antidepressant medication is not always a straightforward process, however, and the patient may have to try out various drugs for a period of weeks or months before finding one that is effective for him or her. In addition, while the SSRIs have comparatively few side effects, such complaints as loss of sexual interest or functioning, nervousness, headaches, gastrointestinal complaints, drowsiness, and insomnia can be significant obstacles to the patient's taking the medication as directed.
Other mainstream approaches
The use of electroconvulsive therapy (ECT), initially introduced in the 1930s, was virtually abandoned as a treatment for MDD for many years, largely as a result of the effectiveness and convenience of psychotropic (mindaltering) medications. Since the 1980s, however, interest in the procedure has renewed; in 1990 the American Psychiatric Association published new guidelines for the use of ECT. Despite media portrayals of ECT as an outdated and cruel form of treatment that causes considerable pain, in actuality the patient is given a sedative and the electrical stimulation is calibrated precisely to produce the maximum therapeutic effects. ECT may be the first line of treatment when a patient cannot tolerate the customary medications or is at high risk of harming themselves; it is more commonly used with patients who fail to respond to drug treatment. In terms of effectiveness, however, ECT actually outperforms medications even among patients who are helped by antidepressants, as well as those who are resistant to drug treatment.
The use of phototherapy ( light therapy ) has proven to be the treatment of choice for patients diagnosed with seasonal affective disorder. Although the reasons for the effectiveness of phototherapy are not yet clear, treatment involves exposing the eyes to bright (2,500 lux) light for several minutes a day. Currently, however, there is little evidence to suggest that phototherapy is useful in the treatment of other types of MDD.
Alternative and complementary treatments
The National Center for Complementary and Alternative Medicine (NCCAM) is conducting an ongoing series of clinical tests of alternative and complementary treatments for depression. Those that have been shown to reduce symptoms of depression and compare favorably with conventional treatments include acupuncture ; Ayurvedic medicine; meditation ; and a therapeutic diet designed to be free of caffeine and refined sugar.
Herbal preparations are common alternative treatments for depression; in fact an NCCAM study found that depression is the single most common reason for people in the United States to purchase herbal remedies. Some, such as St. John's wort, have been used in Europe for decades. The German Commission E, which regulates government approval of herbal preparations in German-speaking Europe, recently approved the use of Gingko biloba extract as a treatment for depression. The most important caution is that persons who are using herbal remedies, whether to treat depression or other conditions, should always tell their doctor what they are taking, how much, and how often . This warning is crucial because some herbal preparations that are safe in themselves can interact with prescription medications. In particular, St. John's wort has been reported to cause interactions with fluoxetine (Prozac).
Some complementary approaches appear to be helpful to persons with depression because they offer pleasurable experiences for the senses or lift the person's spirit. These include aromatherapy ; music therapy; pet therapy; humor; therapeutic massage; and yoga .
Prognosis
Major depression is increasingly viewed as a chronic condition for many people. Left untreated, a depressive episode may last four months or longer, regardless of the age of onset. While most people recover fully from a given depressive episode, eventual recurrence is common. Long-term studies of people with MDD indicate that about 60% of patients who have one episode of depression will have a second episode; with each succeeding episode, the chances of a subsequent episode increase. For example, persons having a third episode stand a 90% chance of having a fourth. Between depressive episodes, the patient's mood may return to a nondepressed state (in about two-thirds of the cases) or continue to show some degree of impairment (one-third of cases). Patients who recover only partially between episodes appear to be at especially high risk of recurrence.
Community studies indicate that about 60% of the people diagnosed with MDD are greatly improved or fully recovered by one year after diagnosis. A very severe initial episode of depression, the presence of a coexisting dysthymic disorder , or the existence of a serious medical condition are associated with a poorer prognosis.
Prevention
While programs specifically aimed at preventing MDD are not widespread, early interventions with children to address some of the issues related to depression have met with success. In particular, social skills training has been found to reduce symptoms of depression, perhaps by enabling children to develop the kinds of social supports and friendships that promote good mental health. Cognitive behavioral techniques that teach people to challenge dysfunctional thought patterns, such as the tendency to deny responsibility for good outcomes and to feel overly responsible for negative events, has been found to successfully reduce the rates of depressive symptoms in children and college students. In addition, psychoeducational work with parents having mood disorders has been effective in improving the adjustment of their children. Long-term follow-up of such approaches is incomplete, but these studies support the possibility that improved individual and family functioning may help to lower rates of depression in the future.
As the factors that increase an individual's vulnerability to depression become better understood, effective strategies for early intervention and possible prevention become possible. Brief therapies that target such symptoms as maladaptive thought patterns or interpersonal problems may lower the risk of serious mood disturbances. Knowledge of the mental health implications of natural or humanly caused disasters has already resulted in much improved mental health services to communities in need. It is realistic to expect that appropriate treatment will become more available and accessible to people experiencing less dramatic setbacks to their ability to function in the future.
See also Adjustment disorder ; ; ; Creative therapies ; Family psychoeducation ; Genetic factors and mental disorders ; Grief
Resources
BOOKS
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th edition, text revised. Washington, DC: American Psychiatric Association,2000.
Beck, Aaron T., M.D., and others. Cognitive Therapy of Depression. New York: Guilford Press, 1979.
Ingram, Rick E. and Joseph M. Price, eds. Vulnerability to Psychopathology; Risk Across the Lifespan. New York: Guilford Press, 2001.
Martell, Christopher, and others. Depression in Context: Strategies for Guided Action. New York: W. W. Norton,2001.
McCullough, James P., Ph.D. Treatment for Chronic Depression. New York: Guilford Press, 2000.
Pelletier, Kenneth R., MD. "CAM Therapies for Specific Conditions: Depression." The Best Alternative Medicine. Part II. New York: Simon and Schuster, 2002.
Rush, John A., ed. Mood and Anxiety Disorders. Philadephia: Williams and Wilkins, 1998.
Seligman, Martin E. P., Ph.D. Helplessness: On Depression, Development, and Death. San Francisco: Freeman, 1975.
Simonds, Susan L. Depression and Women: An Integrative Treatment Approach. New York: Springer Publishing Company, 2001.
Steiner, Meir, M.D. and others, eds. Mood Disorders in Women. London: Martin Dunitz Limited, 2000.
PERIODICALS
Brodaty, H. and others. "A 25-year Longitudinal Comparison Study of the Outcome of Depression." Psychological Medicine 31 (2001): 1347-1358.
Nolan, Carla L., and others. "Prefrontal Cortical Volume in Childhood-Onset Major Depression." Archives of General Psychiatry 59 (2002): 173-175.
Nuland, Sherwin B., M.D. "The Uncertain Art: Lightning On My Mind." The American Scholar 71 (Spring 2002): 127-131.
ORGANIZATIONS
American Academy of Child and Adolescent Psychiatry. 3615 Wisconsin Avenue, NW, Washington, DC 20016. (202) 966-7300. <www.aacap.org> .
National Depressive and Manic-Depressive Association. 730 North Franklin Street, Suite 501, Chicago, IL 60610-3526. (800) 826-3632. <www.ndmda.org> .
OTHER
National Center for Complementary and Alternative Medicine (NCCAM) Clearinghouse. P.O. Box 7923, Gaithersburg, MD 20898. (888) 644-6226. TTY: (866) 464-3615. Fax:(866) 464-3616. <www.nccam.nih.gov> .
National Institute of Mental Health (NIMH). Depression in Children and Adolescents: A Fact Sheet for Physicians. <www.nimh.nih.gov/publicat/depchildresfact.cfm> .
Jane A. Fitzgerald, Ph.D.
plz guide me