Dementia

Definition
Dementia is not a specific disorder or disease. It is a syndrome (group of symptoms) associated with a progressive loss of memory and other intellectual functions that is serious enough to interfere with performing the tasks of daily life. Dementia can occur to anyone at any age from an injury or from oxygen deprivation, although it is most commonly associated with aging. It is the leading cause of institutionalization of older adults.
Description
The definition of dementia has become more inclusive over the past several decades. Whereas earlier descriptions of dementia emphasized memory loss, the last three editions of the professional's diagnostic handbook, Diagnostic and Statistical Manual of Mental Disorders (also known as the DSM ) define dementia as an overall decline in intellectual function, including difficulties with language, simple calculations, planning and judgment, and motor (muscular movement) skills as well as loss of memory. Although dementia is not caused by aging itself— most researchers regard it as resulting from injuries, infections, brain diseases, tumors, or other disorders— it is quite common in older people. The prevalence of dementia increases rapidly with age; it doubles every five years after age 60. Dementia affects only 1% of people aged 60–64 but 30%–50% of those older than 85. About four to five million persons in the United States are affected by dementia as of 2002. Surveys indicate that dementia is the condition most feared by older adults in the United States.
Causes and symptoms
Causes
Dementia can be caused by nearly forty different diseases and conditions, ranging from dietary deficiencies and metabolic disorders to head injuries and inherited diseases. The possible causes of dementia can be categorized as follows:
- Primary dementia. These dementias are characterized by damage to or wasting away of the brain tissue itself. They include Alzheimer's disease (AD), frontal lobe dementia (FLD), and Pick's disease. FLD is dementia caused by a disorder (usually genetic) that affects the front portion of the brain, and Pick's disease is a rare type of primary dementia that is characterized by a progressive loss of social skills, language, and memory, leading to personality changes and sometimes loss of moral judgment.
- Multi-infarct dementia (MID). Sometimes called vascular dementia , this type is caused by blood clots in the small blood vessels of the brain. When the clots cut off the blood supply to the brain tissue, the brain cells are damaged and may die. (An infarct is an area of dead tissue caused by obstruction of the circulation.)
- Lewy body dementia. Lewy bodies are areas of injury found on damaged nerve cells in certain parts of the brain. They are associated with Alzheimer's and Parkinson's disease, but researchers do not yet know whether dementia with Lewy bodies is a distinct type of dementia or a variation of Alzheimer's or Parkinson's disease.
- Dementia related to alcoholism or exposure to heavy metals (arsenic, antimony, bismuth).
- Dementia related to infectious diseases. These infections may be caused by viruses (HIV, viral encephalitis); spirochetes (Lyme disease, syphilis); or prions (Creutzfeldt-Jakob disease). Spirochetes are certain kinds of bacteria, and prions are protein particles that lack nucleic acid.
- Dementia related to abnormalities in the structure of the brain. These may include a buildup of spinal fluid in the brain (hydrocephalus); tumors; or blood collecting beneath the membrane that covers the brain (subdural hematoma).
Dementia may also be associated with depression, low levels of thyroid hormone, or niacin or vitamin B 12 deficiency. Dementia related to these conditions is often reversible.
Genetic factors in dementia
Genetic factors play a role in several types of dementia, but the importance of these factors in the development of the dementia varies considerably. Alzheimer's disease (AD) is known, for example, to have an autosomal (non-sex-related) dominant pattern in most early-onset cases as well as in some late-onset cases, and to show different degrees of penetrance (frequency of expression) in late-life cases. Moreover, researchers have not yet discovered how the genes associated with dementia interact with other risk factors to produce or trigger the dementia. One non-genetic risk factor presently being investigated is toxic substances in the environment.
EARLY-ONSET ALZHEIMER'S DISEASE. In early-onset AD, which accounts for 2%–7% of cases of AD, the symptoms develop before age 60. It is usually caused by an inherited genetic mutation. Early-onset AD is also associated with Down syndrome, in that persons with trisomy 21 (three forms of human chromosome 21 instead of a pair) often develop early-onset AD.
LATE-ONSET ALZHEIMER'S DISEASE. Recent research indicates that late-onset Alzheimer's disease is a polygenic disorder; that is, its development is influenced by more than one gene. It has been known since 1993 that a specific form of a gene (the APOE gene) on human chromosome 19 is a genetic risk factor for late-onset AD. In 1998 researchers at the University of Pittsburgh reported on another gene that controls the production of bleomycin hydrolase (BH) as a second genetic risk factor that acts independently of the APOE gene. In December 2000, three separate research studies reported that a gene on chromosome 10 that may affect the processing of a protein (called amyloid-beta protein) is also involved in the development of late-onset AD. When this protein is not properly broken down, a starchy substance builds up in the brains of people with AD to form the plaques that are characteristic of the disease.
MULTI-INFARCT DEMENTIA (MID). While the chief risk factors for MID are high blood pressure, advanced age, and male sex, there is an inherited form of MID called CADASIL, which stands for cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy. CADASIL can cause psychiatric disturbances and severe headaches as well as dementia.
FRONTAL LOBE DEMENTIAS. Researchers think that between 25% and 50% of cases of frontal lobe dementia involve genetic factors. Pick's dementia appears to have a much smaller genetic component than FLD. It is not yet known what other risk factors combine with inherited traits to influence the development of frontal lobe dementias.
FAMILIAL BRITISH DEMENTIA (FBD). FBD is a rare autosomal dominant disorder that was first reported in the 1940s in a large British family extending over nine generations. FBD resembles Alzheimer's in that the patient develops a progressive dementia related to amyloid deposits in the brain. In 1999, a mutated gene that produces the amyloid responsible for FBD was discovered on human chromosome 13. Studies of this mutation may yield further clues to the development of Alzheimer's disease as well as FBD itself.
CREUTZFELDT-JAKOB DISEASE. Although Creutzfeldt-Jakob disease is caused by a prion, researchers think that 5%–15% of cases may have a genetic component.
Symptoms
The fourth edition, text revised version of the DSM was published in 2000, and is known as DSM-IV-TR . DSM-IV-TR identifies certain symptoms as criteria that must be met for a patient to be diagnosed with dementia. One criterion is significant weakening of the patient's memory with regard to learning new information as well as recalling previously learned information. In addition, the patient must be found to have one or more of the following disturbances:
- Aphasia. Aphasia refers to loss of language function. A person with dementia may use vague words like "it" or "thing" often because he or she can't recall the exact name of an object; the affected person may echo what other people say, or repeat a word or phrase over and over. People in the later stages of dementia may stop speaking at all.
- Apraxia. Apraxia refers to loss of the ability to perform intentional movements even though the person is not paralyzed, has not lost the sense of touch, and knows what he or she is trying to do. For example, a patient with apraxia may stop brushing their teeth, or have trouble tying their shoelaces.
- Agnosia. Agnosia refers to loss of the ability to recognize objects even though the person's sight and sense of touch are normal. People with severe agnosia may fail to recognize family members or even their own face reflected in a mirror.
- Problems with abstract thinking and complex behavior. This criterion refers to the loss of the ability to make plans, carry out the steps of a task in the proper order, make appropriate decisions, evaluate situations, show good judgment, etc. For example, a patient might light a stove burner under a saucepan before putting food or water in the pan, or be unable to record checks and balance their checkbook.
DSM-IV-TR also specifies that these disturbances must be severe enough to cause problems in the person's daily life, and that they must represent a decline from a previously higher level of functioning.
In addition to the changes in cognitive functioning, the symptoms of dementia may also include personality changes and emotional instability. Patients with dementia sometimes become mildly paranoid because their loss of short-term memory leads them to think that mislaid items have been stolen. About 25% of patients with dementia develop a significant degree of paranoia , that is, generalized suspiciousness or specific delusions of persecution. Mood swings, anxiety, and irritability or anger are also frequent occurrences, particularly when patients with dementia are in situations that force them to recognize the extent of their impairment.
The following sections describe the signs and symptoms that are used to differentiate among the various types of dementia during a diagnostic evaluation.
ALZHEIMER'S DISEASE. Dementia related to AD often progresses slowly; it may be accompanied by irritability, wide mood swings, and personality changes in the early stage. Many patients, however, retain their normal degree of sociability in the early stages of Alzheimer's. In second-stage AD, the patient typically gets lost easily, is
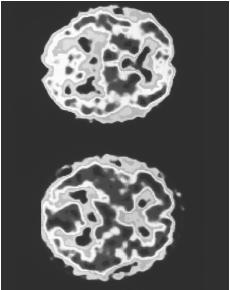
MULTI-INFARCT DEMENTIA. In MID, the symptoms are more likely to occur after age 70. In the early stages, the patient retains his or her personality more fully than a patient with AD. Another distinctive feature of this type of dementia is that it often progresses in a stepwise fashion; that is, the patient shows rapid changes in functioning, then remains at a plateau for a while rather than showing a continuous decline. The symptoms of MID may also have a "patchy" quality; that is, some of the patient's mental functions may be severely affected while others are relatively undamaged. Other symptoms of MID include exaggerated reflexes, an abnormal gait (manner of walking), loss of bladder or bowel control, and inappropriate laughing or crying.
DEMENTIA WITH LEWY BODIES. This type of dementia may combine some features of AD, such as severe memory loss and confusion, with certain symptoms associated with Parkinson's disease, including stiff muscles, a shuffling gait, and trembling or shaking of the hands. Visual hallucinations may be one of the first symptoms of dementia with Lewy bodies.
FRONTAL LOBE DEMENTIAS. The frontal lobe dementias are gradual in onset. Pick's dementia is most likely to develop in persons between 40 and 60, while FLD typically begins before the age of 65. The first symptoms of the frontal lobe dementias often include socially inappropriate behavior (rude remarks, sexual acting-out, disregard of personal hygiene, etc.). Patients are also often obsessed with eating and may put non-food items in their mouths as well as making frequent sucking or smacking noises. In the later stages of frontal lobe dementia or Pick's disease, the patient may develop muscle weakness, twitching, and delusions or hallucinations.
CREUTZFELDT-JAKOB DISEASE. The dementia associated with Creutzfeldt-Jakob disease occurs most often in persons between 40 and 60. It is typically preceded by a period of several weeks in which the patient complains of unusual fatigue , anxiety, loss of appetite, or difficulty concentrating. This type of dementia also usually progresses much more rapidly than other dementias, frequently over a span of a few months.
Demographics
The demographic distribution of dementia varies somewhat according to its cause. Moreover, recent research indicates that dementia in many patients has overlapping causes, so that it is not always easy to assess the true rates of occurrence of the different types. For example, AD and MID are found together in about 15%–20% of cases.
Alzheimer's disease
AD is by far the most common cause of dementia in the elderly, accounting for 60%–80% of cases. It is estimated that four million adults in the United States suffer from AD. The disease strikes women more often than men, but researchers don't know yet whether the sex ratio simply reflects the fact that women in developed countries tend to live longer than men, or whether female sex is itself a risk factor for AD. One well-known long-term study of Alzheimer's in women is the Nun Study, begun in 1986 and presently conducted at the University of Kentucky.
Multi-infarct dementia
MID is responsible for between 15% and 20% of cases of dementia (not counting cases in which it coexists with AD). Unlike AD, MID is more common in men than in women. Diabetes, high blood pressure, a history of smoking, and heart disease are all risk factors for MID. Researchers in Sweden have suggested that MID is underdiagnosed, and may coexist with other dementias more frequently than is presently recognized.
Dementia with Lewy bodies
Dementia with Lewy bodies is now thought to be the second most common form of dementia after Alzheimer's disease. But because researchers don't completely understand the relationship between Lewy bodies, AD, and Parkinson's disease, the demographic distribution of this type of dementia is also unclear.
Other dementias
FLD, Pick's disease, Huntington's disease, Parkinson's disease, HIV infection, alcoholism, head trauma, etc. account for about 10% of all cases of dementia. In FLD and Pick's dementia, women appear to be affected slightly more often than men.
Diagnosis
In some cases, a patient's primary physician may be able to diagnose the dementia; in many instances, however, the patient will be referred to a neurologist or a gerontologist (specialist in medical care of the elderly). Distinguishing one disorder from other similar disorders is a process called differential diagnosis . The differential diagnosis of dementia is complicated because of the number of possible causes; because more than one cause may be present at the same time; and because dementia can coexist with such other conditions as depression and delirium . Delirium is a temporary disturbance of consciousness marked by confusion, restlessness, inability to focus one's attention, hallucinations, or delusions. In elderly people, delirium is frequently a side effect of surgery, medications, infectious illnesses, or dehydration. Delirium can be distinguished from dementia by the fact that delirium usually comes on fairly suddenly (in a few hours or days) and may vary in severity— it is often worse at night. Dementia develops much more slowly, over a period of months or years, and the patient's symptoms are relatively stable. It is possible for a person to have delirium and dementia at the same time.
Another significant diagnostic distinction in elderly patients is the distinction between dementia and ageassociated memory impairment (AAMI), which is sometimes called benign senescent forgetfulness. Older people with AAMI have a mild degree of memory loss; they do not learn new information as quickly as younger people, and they may take longer to recall a certain fact or to balance their checkbook. But they do not suffer the degree of memory impairment that characterizes dementia, and they do not get progressively worse.
Clinical interview
The doctor will begin by taking a full history, including the patient's occupation and educational level as well as medical history. The occupational and educational history allows the examiner to make a more accurate assessment of the extent of the patient's memory loss and other evidence of intellectual decline. In some cases, the occupational history may indicate exposure to heavy metals or other toxins. A complete medical history allows the doctor to assess such possibilities as delirium, depression, alcohol-related dementia, dementia related to head injury, or dementia caused by infection. It is particularly important for the doctor to have a list of all the patient's medications, including over-the-counter and alternative herbal preparations, because of the possibility that the patient's symptoms are related to side effects of these substances.
Whenever possible, the examiner will consult the patient's family members or close friends as part of the history-taking process. In many cases, friends and relatives can provide more detailed information about the patient's memory problems and loss of function.
Mental status examination
A mental status examination (MSE) evaluates the patient's ability to communicate, follow instructions, recall information, perform simple tasks involving movement and coordination, as well as his or her emotional state and general sense of space and time. The MSE includes the doctor's informal evaluation of the patient's appearance, vocal tone, facial expressions, posture, and gait as well as formal questions or instructions. A common form that has been used since 1975 is the so-called Folstein Mini-Mental Status Examination, or MMSE. Questions that are relevant to diagnosing dementia include asking the patient to count backward from 100 by 7s, to make change, to name the current President of the United States, to repeat a short phrase after the examiner (such as, "no ifs, ands, or buts"); to draw a clock face or geometric figure, and to follow a set of instructions involving movement (such as, "Show me how to throw a ball" or "Fold this piece of paper and place it under the lamp on the bookshelf.") The examiner may test the patient's abstract reasoning ability by asking him or her to explain a familiar proverb ("People who live in glass houses shouldn't throw stones," for example) or test the patient's judgment by asking about a problem with a common-sense solution, such as what one does when a prescription runs out.
Neurological examination
A neurological examination includes an evaluation of the patient's cranial nerves and reflexes. The cranial nerves govern the ability to speak as well as sight, hearing, taste, and smell. The patient will be asked to stick out the tongue, follow the examiner's finger with the eyes, raise the eyebrows, etc. The patient is also asked to perform certain actions (such as touching the nose with the eyes closed) that test coordination and spatial orientation. The doctor will usually touch or tap certain areas of the body, such as the knee or the sole of the foot, to test the patient's reflexes. Failure to respond to the touch or tap may indicate damage to certain parts of the brain.
Laboratory tests
Blood and urine samples may be collected in order to rule out such conditions as thyroid deficiency, niacin or vitamin B 12 deficiency, heavy metal poisoning, liver disease, HIV infection, syphilis, anemia, medication reactions, or kidney failure. A lumbar puncture (spinal tap) may be done to rule out neurosyphilis.
Diagnostic imaging
The patient may be given a computed tomography (CT) scan or magnetic resonance imaging (MRI) to detect evidence of strokes, disintegration of the brain tissue in certain areas, blood clots or tumors, a buildup of spinal fluid, or bleeding into the brain tissue. Positron-emission tomography (PET) or single-emission computed tomography (SPECT) imaging is not used routinely to diagnose dementia, but may be used to rule out Alzheimer's disease or frontal lobe degeneration if a patient's CT scan or MRI is unrevealing.
Treatments
Reversible and responsive dementias
Some types of dementia are reversible, and a few types respond to specific treatments related to their causes. Dementia related to dietary deficiencies or metabolic disorders is treated with the appropriate vitamins or thyroid medication. Dementia related to HIV infection often responds well to zidovudine (Retrovir), a drug given to prevent the AIDS virus from replicating. Multi-infarct dementia is usually treated by controlling the patient's blood pressure and/or diabetes; while treatments for these disorders cannot undo damage already caused to brain tissue, they can slow the progress of the dementia. Patients with alcohol-related dementia often improve over the long term if they are able to stop drinking. Dementias related to head injuries, hydrocephalus, and tumors are treated by surgery.
It is important to evaluate and treat elderly patients for depression, because the symptoms of depression in older people often mimic dementia. This condition is sometimes called pseudodementia. In addition, patients who suffer from both depression and dementia often show some improvement in intellectual functioning when the depression is treated. The medications most often used for depression related to dementia are the selective serotonin reuptake inhibitors (SSRIs) paroxetine and sertraline . The mental status examination should be repeated after six–12 weeks of antidepressant medication.
Irreversible dementias
As of 2001, there are no medications or surgical techniques that can cure Alzheimer's disease, the frontal lobe dementias, MID, or dementia with Lewy bodies. There are also no "magic bullets" that can slow or stop the progression of these dementias. There is, however, one medication, Aricept, that is being used to halt the progression of Alzheimer's disease. In addition, another medication called galantamine (Reminyl) is also being used to treat the symptoms of Alzheimer's disease. Patients may be given medications to ease the depression, anxiety, sleep disturbances, and other behavioral symptoms that accompany dementia, but most physicians prescribe relatively mild dosages in order to minimize the troublesome side effects of these drugs. Dementia with Lewy bodies appears to respond better to treatment with the newer antipsychotic medications than to treatment with such older drugs as haloperidol (Haldol).
Patients in the early stages of dementia can often remain at home with some help from family members or other caregivers, especially if the house or apartment can be fitted with safety features (handrails, good lighting, locks for cabinets containing potentially dangerous products, nonslip treads on stairs, etc.). Patients in the later stages of dementia, however, usually require skilled care in a nursing home or hospital.
Prognosis
The prognosis for reversible dementia related to nutritional or thyroid problems is usually good once the cause has been identified and treated. The prognoses for dementias related to alcoholism or HIV infection depend on the patient's age and the severity of the underlying disorder.
The prognosis for the irreversible dementias is gradual deterioration of the patient's functioning ending in death. The length of time varies somewhat. Patients with Alzheimer's disease may live from two–20 years with the disease, with an average of seven years. Patients with frontal lobe dementia or Pick's disease live on average between five and 10 years after diagnosis. The course of Creutzfeldt-Jakob disease is much more rapid, with patients living between five and 12 months after diagnosis.
Prevention
The reversible dementias related to thyroid and nutritional disorders can be prevented in many cases by regular physical checkups and proper attention to diet. Dementias related to toxic substances in the workplace may be prevented by careful monitoring of the work environment and by substituting less hazardous materials or substances in manufacturing processes. Dementias caused by infectious diseases are theoretically preventable by avoiding exposure to the prion, spirochete, or other disease agent. Multi-infarct dementia may be preventable in some patients by attention to diet and monitoring of blood pressure. Dementias caused by abnormalities in the structure of the brain are not preventable as of 2002.
With regard to genetic factors, tests are now available for the APOE gene implicated in late-onset Alzheimer's, but these tests are used primarily in research instead of clinical practice. One reason is that the test results are not conclusive; about 20% of people who eventually develop AD do not carry this gene. Another important reason is the ethical implications of testing for a disease that presently has no cure. These considerations may change, however, if researchers discover better treatments for primary dementia, more effective preventive methods, or more reliable genetic markers.
See also
Resources
BOOKS
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th edition, text revised. Washington, DC: American Psychiatric Association, 2000.
"Dementia." The Merck Manual of Diagnosis and Therapy , edited by Mark H. Beers, M.D., and Robert Berkow, M.D. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
Lyon, Jeff, and Peter Gorner. Altered Fates: Gene Therapy and the Retooling of Human Life. New York and London: W. W. Norton & Co., Inc., 1996.
Marcantonio, Edward, M.D. "Dementia." Chapter 40 in The Merck Manual of Geriatrics, edited by Mark H. Beers, M.D., and Robert Berkow, M.D. Whitehouse Station, NJ: Merck Research Laboratories, 2000.
Morris, Virginia. How to Care for Aging Parents. New York: Workman Publishing, 1996. A good source of information about caring for someone with dementia as well as information about dementia itself.
PERIODICALS
"Alzheimer's Disease: Recent Progress and Prospects." Harvard Mental Health Letter (Parts 1, 2, and 3) 18 (October–December 2001).
ORGANIZATIONS
Alzheimer's Association. 919 North Michigan Avenue, Suite 1000, Chicago, IL 60611. (800) 272-3900.
Alzheimer's Disease International. 45/46 Lower Marsh, London SE1 7RG, United Kingdom. (+44 20) 7620 3011. E-mail: adi@alz.co.uk. <www.alz.co.uk> .
National Institute of Mental Health. 6001 Executive Boulevard, Room 8184, MSC 9663, Bethesda, MD 20892-9663. (301) 443-4513. <www.nimh.nih.gov> .
National Institute of Neurological Disorders and Stroke (NINDS). Building 31, Room 8A06, 9000 Rockville Pike, Bethesda, MD 20892. (301) 496-5751. <www.ninds.nih.gov> .
National Institute on Aging Information Center. P.O. Box 8057, Gaithersburg, MD 20898. (800) 222-2225 or (301) 496-1752.
National Organization for Rare Disorders (NORD). P. O. Box 8923, New Fairfield, CT 06812. (800) 447-6673 or (203) 746-6518.
OTHER
Alzheimer's Disease Education and Referral (ADEAR). <www.alzheimers.org> .
The Nun Study. <www.coa.uky.edu/nunnet> .
Rebecca J. Frey, Ph.D.
Thank-you,
April Vert