Detoxification

Definition
Detoxification is a process in which the body is allowed to free itself of a drug. During this period, the symptoms of withdrawal are also treated. Detoxification is the primary step in any drug treatment program, and is used as the initial phase in treating alcohol, heroin, inhalant, sedative, and hypnotic addictions.
Purpose
The goal of detoxification is to clear the toxins out of the body so that the body can adjust and heal itself after being dependent on a substance. In order for the recovering person to stay abstinent on a long-term basis, detoxification needs to lead into long-term community residential program treatment or outpatient drug treatment lasting three to six months.
Precautions
When individuals are physically dependent on a substance, they experience withdrawal symptoms when they abstain from the drug. Withdrawal symptoms vary with each drug of abuse, but can be severe, and even dangerous. Patients who want to overcome their dependence need help managing the withdrawal symptoms. The patient's medical team strives to get the patient off a substance on which he or she is physically dependent, while treating the withdrawal symptoms.
Pregnant women cannot be detoxified from opiates (also called narcotics, including morphine, heroin, and similar drugs) because strict detoxification can increase the risk of spontaneous abortion or premature birth. These women are treated with methadone as an alternative. (Methadone acts as a replacement for the heroin in the woman's body, but the methadone does not provide the "high" that the heroin provides. In addition, methadone is safer for the fetus than heroin.)
In order to be an effective first step of treatment, detoxification must be an individualized process because patients have varying needs.
Description
The body, when allowed to be free from drugs, detoxifies itself through its normal metabolic processes. The withdrawal symptoms are treated during this process so that the patient will be comfortable while the body detoxifies itself.
The process of substance addiction
Before discussing detoxification, it may be useful to understand how the body becomes addicted and why withdrawal symptoms are experienced. In physical addiction or dependence, as a person uses a substance or chemical over a long period of time, his or her body chemistry changes. Once a substance enters the body through drinking, smoking, injecting or inhaling, it travels through the bloodstream to the brain . The brain has a complex reward system built in— when people engage in activities that are important for survival (such as eating), special nerve cells in the brain release chemicals ( neurotransmitters , including dopamine) that induce feelings of pleasure. Because of this reward system in the brain, humans are programmed to want to repeat actions that elicit those pleasant sensations. In other words, feelings of pleasure reinforce certain activities or behaviors. Addictive substances interfere with this reward system. Some drugs mimic the effects of a natural chemical, some block the communication between nerve cells, and some substances trigger a larger-than-normal release of neurotransmitters like dopamine. The result of this interference is that dependent drug users physically need the drug to feel pleasure. As they become more dependent, their bodies becomes less responsive to the substance, and need more of it to get the desired response—a phenomenon called tolerance. Also as a result of the interference with the brain's system, when the dependent user does not have the drug in his or her system, feelings of depression or unpleasant withdrawal symptoms may be experienced. These consequences also reinforce the substance use— people dependent on substances resort to using more drugs to avoid the depression or the withdrawal symptoms.
Withdrawal symptoms
The symptoms and severity of these symptoms vary from one substance to another.
ALCOHOL. After a person who has used alcohol heavily for a long time stops drinking, he or she may experience increased heart rate, shaking, difficulty sleeping, nausea, restlessness, anxiety, and even seizures . The affected person may also experience hallucinations (seeing, hearing, or feeling something that isn't really present). In some cases, delirium tremens (DTs) may occur as part of the withdrawal. Delirium tremens is a violent delirium (fading in and out of consciousness) with tremors, increased motor activity, visual hallucinations, disorientation, confusion, and fever that happens 48-96 hours after the alcohol-dependent person has had his or her last drink. These symptoms can last anywhere from three to 10 days. This state is a medical emergency because it could be fatal.
HEROIN AND OTHER OPIATES. Heroin is part of a family of drugs called opiates or opioids, which are made up of drugs that come from the seeds of the Asian poppy (heroin, opium and morphine, for example) and also manufactured drugs that act like the natural drugs (meperidine or Demerol). Symptoms of opiate withdrawal include restlessness, insomnia , anxiety, irritability, loss of appetite, diarrhea, abdominal cramps, nausea, sweating, chills, and runny eyes and nose.
SEDATIVES AND HYPNOTICS. Sedatives and hypnotics are drug families that are often considered in one group called the sedative-hypnotics. These drugs depress or slow down the body's functions, and can be used to calm anxiety or to induce sleep. When taken in high doses or when abused, these drugs can cause unconsciousness or death. These drugs include barbiturates and benzodiazepines. Some barbiturates are amobarbital (Amytal), pentobarbital (Nembutal), and secobarbital (Seconal). Some benzodiazepines include diazepam (Valium), chlordiazepoxide (Librium), and lorazepam (Ativan). When a person dependent on these drugs stops taking them suddenly, he or she might experience restlessness, muscle cramps, anxiety, insomnia, irritability, paranoid behavior, and even seizures or death.
Alcohol detoxification
Patients being detoxified from alcohol can safely be treated with rest, nutrition, vitamins, and thiamin (a B vitamin whose absorption is affected by alcohol abuse). Detoxification can be completed in an inpatient setting, or patients may participate in intensive outpatient (day hospital) treatment. People with mild or moderate withdrawal symptoms undergo detoxification over a five-day period and receive a benzodiazepine or phenobarbital to help ease the withdrawal symptoms. Delirium tremens can be treated with very high-dose benzodiazepines (such as chlordiazepoxide or diazepam) or with antipsychotic medications such as Haldol ( haloperidol ). The patient usually receives medication at doses high enough to give 60 mg or more of the medication over a 24- to 36-hour period, and the doses of these medications are gradually decreased by 20% each day. Patients who have liver disease, dementia , or patients who are over the age of 65 or with significant medical problems may receive lorazepam for the withdrawal symptoms.
Heroin detoxification
Patients with heroin dependence may receive help with their detoxification in one of two forms. Opioid agonists are drugs that act like heroin in the patient's body but do not provide the same "high," and are given in gradually decreasing doses. Because these medications "act" like heroin, the person does not experience withdrawal symptoms. Some examples of this kind of medication are methadone and levo-alpha-acetylmethadol (LAAM); buprenorphine is a partial opioid agonist, which means that it acts like heroin or methadone, but it limits the effects of opioids so that higher doses produce no greater effects. The second form of help for patients undergoing heroin detoxification is the use of a drug, such as clonidine (Catapres), that blocks some of the withdrawal symptoms. There is also a new method of heroin detoxification called ultra-rapid opioid detoxification under anesthesia/sedation, and there is an experimental method using a medication called lofexidine.
METHADONE SUBSTITUTION. Methadone substitution can occur in outpatient or inpatient settings, and is a method of detoxification that involves helping patients off substances such as heroin by substituting these substances with methadone to ease the withdrawal symptoms, and gradually decreasing the dose until no methadone is needed for the symptoms. Patients may begin with a dose of methadone that is between 20 mg and 40 mg per day. The initial dose may be adjusted so that the most beneficial dose can be discovered, based on the patient's withdrawal symptoms. The dose is then gradually decreased over the next several days. The decrease in methadone dosage is called tapering. If the detoxification is being completed in an inpatient setting, the methadone dose can be tapered more quickly, because medical staff can closely monitor patients for withdrawal, and detoxification can be achieved in about five to 10 days. However, in the case of outpatient detoxification, the taper has to be done much more slowly to assure that the patient does not have an adverse reaction or relapse (use the drug of abuse again) to treat their withdrawal symptoms. The dose may be decreased about 10% per week initially until a dose of 20 mg is reached. Then the dose can be decreased by 3% per week for the rest of the time that the patient needs to be detoxified. Patients are usually comfortable with the slow decrease of the medication until the dose gets below 20 mg/day. At that point, patients tend to become fearful of being off opioids and having symptoms of withdrawal.
Clonidine is used much more frequently than methadone in detoxification. Methadone is used frequently as long-term maintenance treatment for heroin addiction.
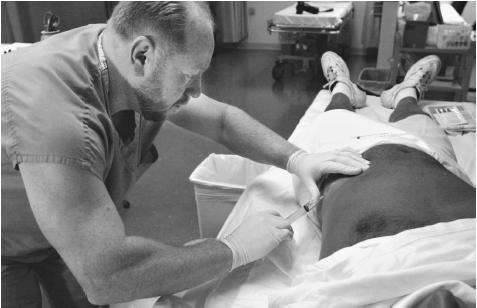
BUPRENORPHINE. Buprenorphine is another medication that is used during opioid detoxification. Because it also acts like heroin in the body, the patient does not experience the withdrawal symptoms as the heroin is being eliminated from the body. It is given as an intramuscular injection or intravenously. It begins to work within 15 minutes and its effects last six hours. A patient receiving buprenorphine receives this medication for at least three days, and then the medication is either gradually withdrawn or discontinued abruptly.
CLONIDINE. Clonidine is a medication that decreases many of the symptoms of opioid withdrawal. Patients may require nonsteroidal anti-inflammatory drugs (NSAIDS, such as ibuprofen) for the treatment of muscle aches. Clonidine's major side effects include sedation and hypotension (low blood pressure). Patients undergoing detoxification using clonidine will have their blood pressure and pulse checked regularly. The starting dose of clonidine is 0.1–0.3 mg every four to six hours— the maximum amount that can be given in one day is 1 mg. During days two through four of the detoxification, the dose of clonidine is adjusted to control the withdrawal symptoms. Again, however, the dose cannot exceed the maximum dose. On the fifth day of detoxification, the dose starts to get slowly tapered.
The clonidine patch is a transdermal patch, meaning that the drug is delivered through the skin and causes the patient to be exposed to a constant amount of the drug over a seven-day period. It also allows the person to experience a more comfortable heroin detoxification. It comes in three doses: 0.1-mg, 0.2-mg, and 0.3-mg. Patients who will use the clonidine patch need to have both the patch on and take oral clonidine during the first two days of the detoxification, because it takes the patch two days to reach a steady state and be effective. The patient takes 0.2 mg of oral clonidine three times a day, and the weight of the patient determines the dose of the patch. On day two, the amount of clonidine that the patient takes by mouth is reduced by half and then it is completely stopped after day three. After seven days, the patch is removed and replaced with a patch that is half the amount of the original dose. The patch is continued for as long as the patient continues to have symptoms of withdrawal. Blood pressure is monitored for the patient using the patch, as well. The detoxification process in general takes about seven days using clonidine.
CLONIDINE-NALTREXONE ULTRA-RAPID DETOXIFICATION. Clonidine-naltrexone ultra-rapid detoxification is a faster means of detoxification than using clonidine alone. The higher the dose of naltrexone that the person receives, the faster he or she can be detoxified. Very close monitoring for withdrawal symptoms is necessary, however, particularly during the first eight hours of the detoxification process. (Naltrexone accelerates the withdrawal.) On the first day of the detoxification process, the patient is premedicated with oxazepam and clonidine. A couple hours later, the patient receives naltrexone. Throughout the rest of the first day, the patient receives oxazepam and clonidine every four to six hours. On the second and third days, the patient receives a larger dose of naltrexone, and continues to receive oxazepam and clonidine throughout the day. After day three, the naltrexone is no longer given, and the patient continues to take the clonidine and oxazepam for two to three more days. Additional medications to help with muscle cramping and nausea may be necessary. In an inpatient setting, the naltrexone can be increased so that the patient can complete detoxification in two to three days.
LOFEXIDINE. Lofexidine is approved for use in England for opioid detoxification. It appears to cause less sedation and fewer cases of low blood pressure than clonidine. In the United States, the National Institute of Drug Abuse (NIDA) is conducting studies on this drug.
ULTRA-RAPID OPIOID DETOXIFICATION UNDER ANESTHESIA/SEDATION. In this new procedure, anesthesia is induced and the patient receives a tracheal tube— a tube in the throat— and a tube in the nose (a nasogastric tube). The patient is given intravenous naloxone or naltrexone through the nasogastric tube. The procedure takes only eight hours and the patient can leave the hospital in one or two days. The patient's withdrawal symptoms are treated with a variety of medications including clonidine, antidiarrheal medications, and benzodiazepines.
Mixed substance abuse
Mixed substance abuse (also called polysubstance abuse) occurs when individuals abuse more than one substance. Many doctors prefer to use phenobarbital to detoxify patients with polysubstance abuse problems. Patients receiving phenobarbital may receive a test dose, and then based on his or her tolerance and symptoms, the dose will be adjusted. Patients cannot receive more than 600 mg of phenobarbital a day. After two to three days, once the patient is doing well, the dose can be reduced by 30-60 mg. Whether detoxification for polysubstance abusers will be completed on an inpatient or outpatient status depends on the drugs the patient abuses.
Benzodiazepines
These medications are often used to help patients during detoxification, but these substances themselves can be abused and addictive. Patients who have taken a prescribed benzodiazepine for two weeks, even in a therapeutic dose, need to be safely detoxified with a slow taper. The amount of drug the person takes is dropped by 10-25% every week if the patient has minimal withdrawal symptoms. If the patient has taken very high doses for long periods of time, he or she is at increased risk for addiction. If the person has been taking a benzodiazepine medication for years, it can take months before he or she can get off the drug. Anticonvulsant medications like carbamazepine (Tegretol) and divalproex sodium (Depakote) can be used to make the detoxification process faster and more comfortable for the patient.
Preparation
The first step in any detoxification, regardless of the substance, is a physical exam and history taken by a physician. This information-gathering and examination will help the treatment team assess the patient's overall health. In general, the healthier the patient is, the better the chances are that the patient will experience a detoxification without serious or life-threatening complications. Patients also need to give urine and blood samples to test for drugs and alcohol.
Aftercare
After the patient has completed detoxification, he or she needs further treatment either at an outpatient, inpatient, residential, or day hospital program in order to remain drug-free for the long term. Patients are treated by trained health care professionals, and some patients are also counseled by people who are recovering from addiction themselves. Many patients also benefit from 12-step programs or self-help groups , such as Alcoholics Anonymous (AA) or Narcotics Anonymous (NA).
Most opioid users are treated with ambulatory or outpatient detoxification or residential treatment followed by outpatient counseling. Some people who have abused opioids and have undergone detoxification and counseling are able to remain drug-free. Many, however, relapse, even after receiving psychotherapy . People recovering from opioid addiction can receive methadone or LAAM as maintenance therapy to prevent relapse. Similar to the aid these medications can give patients during detoxification, when taken daily as a therapy, they continue to "act" as heroin, keeping the withdrawal symptoms from appearing. Methadone maintenance therapy can be provided through either residential or therapeutic communities and outpatient drug-free programs. Methadone maintenance treatment therapy is controversial, however, because it does not cure the person's addiction— it replaces it with another substance. Proponents of methadone maintenance therapy argue that people receiving methadone are able to function much better in society than people addicted to heroin. Because their drug-seeking behavior is reduced, these patients are able to become productive at work and their interpersonal relations improve.
People recovering from alcoholism can also benefit from counseling and support after detoxification, and a maintenance therapy is available to them, as well. Disulfiram (Antabuse) is a medication that interferes with the body's breakdown and processing of alcohol. When alcohol is consumed while a patient is taking disulfiram, the medication makes the effects of the alcohol much worse than the patient would normally experience—facial flushing, headache, nausea and vomiting occurs, even if alcohol is consumed in a small amount. In order for disulfiram to be effective, the patient must want this kind of reinforcement to maintain abstinence and must be committed to it. Patients also must note that any form of alcohol can trigger the undesired effects, including cooking wine or mouthwash with alcohol.
Risks
When benzodiazepines are the drug to which a person is addicted, they have to be discontinued and cannot be given on an outpatient basis because of their potential for abuse. For all patients undergoing detoxification, benzodiazepine use must be monitored carefully because of the potential for new addiction. Elderly patients undergoing detoxification and receiving benzodiazepines must be monitored closely because they are more sensitive to the sedating effects of these drugs, and are also more prone to falls while receiving these drugs. If benzodiazepines are not discontinued gradually, patients can have withdrawal symptoms such as irritability, poor sleep, agitation and seizures. Ultra-rapid opioid detoxification under anesthesia/sedation remains a new and serious procedure. Patients have died receiving this procedure, and this procedure is still being researched.
It should also be noted that many of the substances used in detoxification can themselves cause addictions. An example of this risk has already been given with benzodiazepines—these medications ease withdrawal symptoms during detoxification, but patients can get addicted to these medications, as well.
Normal results
Normal results for a well-managed detoxification would include freedom from the drug of addiction and ability to enter long-term treatment.
Success rates vary among people recovering from substance abuse. As might be expected, patients who successfully complete a full treatment program after detoxification (that includes counseling, psychotherapy, family therapy , and/or group therapy or some combination of those therapy types) achieve higher rates of success at remaining drug-free. Patients who were addicted for shorter periods of time and patients who spend longer periods in treatment are generally more successful at remaining abstinent from drugs over the long term.
Studies indicate that people who abuse alcohol and who want to stop have a higher chance of success if they undergo inpatient detoxification versus outpatient detoxification.
Abnormal results
One abnormal result that may occur is that patients who received nasogastric or tracheal tubes for opioid detoxification under anesthesia may experience adverse effects or complications. These patients are at risk for: trauma to their lips, vocal cords, larynx, teeth; nose bleeds; high blood pressure; elevated heart rate; irregular heartbeat; and vomiting, which can lead to aspiration pneumonia.
An additional abnormal result would be a new addiction as a consequence of the detoxification.
After the detoxification is completed, patients may relapse. Support is critical for patients to continue long-term therapy and successfully overcome addiction.
See also Addiction ; Disease concept of chemical dependency ;
Resources
BOOKS
Beers, Mark H., M.D., and Robert Berkow, M.D., eds. "Alcoholism." The Merck Manual of Diagnosis and Therapy. 17th edition. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
Jaffe, Jerome H., M.D., and others. "Substance-Related Disorders." In Comprehensive Textbook of Psychiatry, edited by Benjamin J. Sadock, M.D. and Virginia A. Sadock, M.D. 7th edition. Philadelphia: Lippincott Williams and Wilkins, 2000.
Matthews, John. "Substance-Related Disorders: Cocaine and Narcotics." In Psychiatry Update and Board Preparation, edited by Thomas A. Stern, M.D. and John B. Herman, M.D. New York: McGraw Hill, 2000.
PERIODICALS
Fuller, Richard K., M.D. and Susanne Hiller-Sturmhofel, Ph.D. "Alcoholism Treatment in the United States: An Overview." Alcohol Research and Health 23 (1999): 69-77.
Khantzian, Edward J., M.D. "Methadone Treatment for Opioid Dependence." American Journal of Psychiatry November 2000: 1895-1896.
Leshner, Alan Ph.D. "Heroin Abuse and Addiction." National Institute on Drug Abuse Research Report Series. NIH Publication Number 00-4165, Washington, D.C. Supt.of doc. US. Govt. Print. Off., 2000.
Shreeram, S. S., M.D., and others. "Psychosis After Ultrarapid Opiate Detoxification." American Journal of Psychiatry June 2001: 970.
ORGANIZATIONS
The College on Problems of Drug Dependency (CPDD). CPDD Executive Offices, Department of Pharmacology, 3420 N.Broad Street,Philadephia, PA,19140. (215) 707-3242. <http://views.vcu.edu/cpdd> .
Institute for Comprehensive Detoxification and Rehabilitation. (877) 704-ICDR (4237). <http://www.views.vcu.edu/cpdd/> .
National Institute on Alcohol Abuse and Alcoholism (NIAAA). 6000 Executive Boulevard, Willco Building, Bethesda, MD, 20892-7003. <http://www.niaaa.nih.gov> .
National Institute on Drug Abuse (NIDA). 6001 Executive Boulevard, Room 5213, Bethesda, MD, 20892-9561. (301) 443-1124. <http://www.nida.nih.gov> .
Susan Hobbs, M.D.