Post-traumatic stress disorder

Definition
Post-traumatic stress disorder, often abbreviated as PTSD, is a complex disorder in which the affected person's memory, emotional responses, intellectual processes, and nervous system have all been disrupted by one or more traumatic experiences. It is sometimes summarized as "a normal reaction to abnormal events." The DSM-IV-TR (the professional's diagnostic manual) classifies PSTD as an anxiety disorder.
Description
PTSD has a unique position as the only psychiatric diagnosis (along with acute stress disorder ) that depends on a factor outside the individual, namely, a traumatic stressor. A patient cannot be given a diagnosis of PTSD unless he or she has been exposed to an event that is considered traumatic. These events include such obvious traumas as rape, military combat, torture, genocide, natural disasters, and transportation or workplace disasters. In addition, it is now recognized that repeated traumas or such traumas of long duration as child abuse , domestic violence, stalking, cult membership, and hostage situations may also produce the symptoms of PTSD in survivors.
A person suffering from PTSD experiences flashbacks, nightmares, or daydreams in which the traumatic event is experienced again. The person may also experience abnormally intense startle responses, insomnia , and may have difficulty concentrating. Trauma survivors with PTSD have been effectively treated with group therapy or individual psychological therapy, and other therapies have helped individuals, as well. Some affected individuals have found support groups or peer counseling groups helpful. Treatment may require several years, and in some cases, PTSD may affect a person for the rest of his or her life.
Demographics
General United States population
PTSD is much more widespread in the general population than was thought when it was first introduced as a diagnostic category. The National Comorbidity Survey, a major epidemiological study conducted between 1990 and 1992, estimates that the lifetime prevalence among adult Americans is 7.8%, with women (10.4%) twice as likely as men (5%) to be diagnosed with PTSD at some point in their lives. These figures represent only a small proportion of adults who have experienced at least one traumatic event—60.7% of men and 51.2% of women respectively. More than 10% of the men and 6% of the women reported experiencing four or more types of trauma in their lives. The most frequently mentioned traumas are:
- witnessing someone being badly hurt or killed
- involvement in a fire, flood, earthquake, severe hurricane, or other natural disaster
- involvement in a life-threatening accident (workplace explosion or transportation accident)
- military combat
The traumatic events most frequently mentioned by men diagnosed with PTSD are rape, combat exposure, childhood neglect , and childhood physical abuse. For women diagnosed with PTSD, the most common traumas are rape, sexual molestation, physical attack, being threatened with a weapon, and childhood physical abuse.
High-risk populations
Some subpopulations in the United States are at greater risk of developing PTSD. The lifetime prevalence of PTSD among persons living in depressed urban areas or on Native American reservations is estimated at 23%. For victims of violent crimes, the estimated rate is 58%.
Military veterans
Information about PTSD in veterans of the Vietnam era is derived from the National Vietnam Veterans Readjustment Survey (NVVRS), conducted between 1986 and 1988. The estimated lifetime prevalence of PTSD among American veterans of this war is 30.9% for men and 26.9% for women. An additional 22.5% of the men and 21.2% of the women have been diagnosed with partial PTSD at some point in their lives. The lifetime prevalence of PTSD among veterans of World War II and the Korean War is estimated at 20%.
Cross-cultural issues
Further research needs to be done on the effects of ethnicity and culture on post-traumatic symptoms. As of 2001, most PTSD research has been done by Western clinicians working with patients from a similar background. Researchers do not yet know whether persons from non-Western societies have the same psychological reactions to specific traumas or whether they develop the same symptom patterns.
Causes and symptoms
Causes
When PTSD was first suggested as a diagnostic category for DSM-III in 1980, it was controversial precisely because of the central role of outside stressors as causes of the disorder. Psychiatry has generally emphasized the internal weaknesses or deficiencies of individuals as the source of mental disorders; prior to the 1970s, war veterans, rape victims, and other trauma survivors were often blamed for their symptoms and regarded as cowards, moral weaklings, or masochists. The high rate of psychiatric casualties among Vietnam veterans, however, led to studies conducted by the Veterans Administration. These studies helped to establish PTSD as a legitimate diagnostic entity with a complex set of causes.
BIOCHEMICAL/PHYSIOLOGICAL CAUSES. Present neurobiological research indicates that traumatic events cause lasting changes in the human nervous system, including abnormal secretions of stress hormones. In addition, in PTSD patients, researchers have found changes in the amygdala and the hippocampus—the parts of the brain that form links between fear and memory. Experiments with ketamine, a drug that inactivates one of the neurotransmitter chemicals in the central nervous system, suggest that trauma works in a similar way to damage associative pathways in the brain. Positron emission tomography (PET) scans of PTSD patients suggest that trauma affects the parts of the brain that govern speech and language.
SOCIOCULTURAL CAUSES. Studies of specific populations of PTSD patients (combat veterans, survivors of rape or genocide, former political hostages or prisoners, etc.) have shed light on the social and cultural causes of PTSD. In general, societies that are highly authoritarian, glorify violence, or sexualize violence have high rates of PTSD even among civilians.
OCCUPATIONAL FACTORS. Persons whose work exposes them to traumatic events or who treat trauma survivors may develop secondary PTSD (also known as compassion fatigue or burnout). These occupations include specialists in emergency medicine, police officers, firefighters, search-and-rescue personnel, psychotherapists, disaster investigators, etc. The degree of risk for PTSD is related to three factors: the amount and intensity of exposure to the suffering of trauma victims; the worker's degree of empathy and sensitivity; and unresolved issues from the worker's personal history.
PERSONAL VARIABLES. Although the most important causal factor in PTSD is the traumatic event itself, individuals differ in the intensity of their cognitive and emotional responses to trauma; some persons appear to be more vulnerable than others. In some cases, this greater vulnerability is related to temperament or natural disposition, with shy or introverted people being at greater risk. In other cases, the person's vulnerability results from chronic illness, a physical disability, or previous traumatization—particularly abuse in childhood. As of 2001, researchers have not found any correlation between race and biological vulnerability to PTSD.
Symptoms
DSM-IV-TR specifies six diagnostic criteria for PTSD:
- Traumatic stressor: The patient has been exposed to a catastrophic event involving actual or threatened death or injury, or a threat to the physical integrity of the self or others. During exposure to the trauma, the person's emotional response was marked by intense fear, feelings of helplessness, or horror. In general, stressors caused intentionally by human beings (genocide, rape, torture, abuse, etc.) are experienced as more traumatic than accidents, natural disasters, or "acts of God."
- Intrusive symptoms: The patient experiences flashbacks, traumatic daydreams, or nightmares, in which he or she relives the trauma as if it were recurring in the present. Intrusive symptoms result from an abnormal process of memory formation. Traumatic memories have two distinctive characteristics: 1) they can be triggered by stimuli that remind the patient of the traumatic event; 2) they have a "frozen" or wordless quality, consisting of images and sensations rather than verbal descriptions.
- Avoidant symptoms: The patient attempts to reduce the possibility of exposure to anything that might trigger memories of the trauma, and to minimize his or her reactions to such memories. This cluster of symptoms includes feeling disconnected from other people, psychic numbing, and avoidance of places, persons, or things associated with the trauma. Patients with PTSD are at increased risk of substance abuse as a form of self-medication to numb painful memories.
- Hyperarousal: Hyperarousal is a condition in which the patient's nervous system is always on "red alert" for the return of danger. This symptom cluster includes hypervigilance, insomnia, difficulty concentrating, general irritability, and an extreme startle response. Some clinicians think that this abnormally intense startle response may be the most characteristic symptom of PTSD.
- Duration of symptoms: The symptoms must persist for at least one month.
- Significance: The patient suffers from significant social, interpersonal, or work-related problems as a result of the PTSD symptoms. A common social symptom of PTSD is a feeling of disconnection from other people (including loved ones), from the larger society, and from spiritual or other significant sources of meaning.
Diagnosis
The diagnosis of PTSD is complicated by several factors.
Time of onset/symptom duration
In the case of a known trauma of recent occurrence—most often a civilian disaster or war—the diagnosis of PTSD is relatively straightforward, based on the criteria listed above.
DSM-IV introduced a new diagnostic category, acute stress disorder, to differentiate between time-limited and longer-term stress reactions. In acute stress disorder, the hyperarousal and intrusive symptoms last between two days and four weeks. If the symptoms last beyond four weeks, and all of the above criteria are met, the diagnosis is changed to PTSD.
The diagnosis of PTSD is more difficult in cases of delayed reaction to trauma. Some individuals do not develop symptoms of PTSD until months or even years after the traumatic event. DSM-IV-TR specifies an interval of at least six months between the event and the development of symptoms for a diagnosis of PTSD with delayed onset. Delayed symptoms are often triggered by a situation that resembles the original trauma, as when a person raped in childhood experiences workplace sexual harassment.
Individual variations in response to stressors
DSM-III and its successors included the category of adjustment disorder to differentiate abnormal reactions to such painful but relatively common life events ("ordinary stressors") as divorce, job loss, or bereavement from symptoms resulting from overwhelming trauma. The differential diagnosis (the process of determining that the diagnosis is one disorder although it may resemble another) is complicated, however, by the fact that "ordinary stressors" sometimes reawaken unresolved childhood trauma, producing the delayed-reaction variant of PTSD.
Dual diagnoses
Most patients with PTSD (as many as 80%) have been diagnosed with one of the anxiety (30–60%), dissociative, mood (26–85%), or somatoform disorders as well as with PTSD. Between 40–60% of persons with delayed-reaction PTSD are diagnosed with a personality disorder, most often borderline personality disorder . Another common dual diagnosis is PTSD/substance abuse disorder. Between 60%–80% of patients who develop PTSD turn to alcohol or narcotics in order to avoid or numb painful memories. According to the NVVRS, the estimated lifetime prevalence of alcohol abuse among male Vietnam veterans is 39.2%, and the estimated lifetime prevalence of drug abuse is 5.7%. Dual diagnoses complicate treatment because the therapist
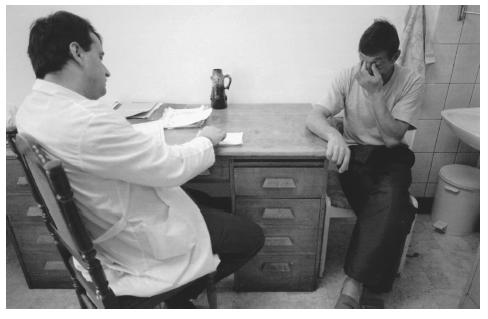
Psychological measures
As of 2002, there are no physical tests to establish a diagnosis of PTSD. The diagnosis is usually made on the basis of the patient's history and results from one or more short-answer interviews or symptom inventories. The instruments most often used to evaluate patients for PTSD include the Anxiety Disorders Interview Scale (ADIS), the Beck Depression Inventory , the Clinician-Administered PTSD Scale (CAPS), the Disorders of Extreme Stress Inventory (DESI), the Dissociative Experiences Scale (DES), the Hamilton Anxiety Scale , and the Impact of Event Scale (IES).
Treatments
Psychological and social interventions
In general, there have been few well-controlled clinical trials of treatment options for PTSD, particularly for severely affected patients.
Critical incident stress debriefing (CISD) is a treatment offered to patients within 48 hours following a civilian disaster or war zone trauma. It is intended to weaken the acute symptoms of the trauma and to forestall the development of full-blown PTSD. CISD usually consists of four phases:
- description of the traumatic event
- sharing of survivors' emotional reactions to the event
- open discussion of symptoms caused by the event
- reassurance that the symptoms are normal responses to trauma, followed by discussion of coping strategies
Critical incident stress management is a system of interventions designed to help emergency/disaster response workers, public safety personnel, and therapists deal with stress reactions before they develop secondary PTSD.
Other mainstream treatment methods used with patients who have already developed PTSD include:
- Cognitive-behavioral therapy . There are two treatment approaches to PTSD included under this heading: exposure therapy, which seeks to desensitize the patient to reminders of the trauma; and anxiety management training, which teaches the patient strategies for reducing anxiety. These strategies may include relaxation training, biofeedback , social skills training , distraction techniques, or cognitive restructuring.
- Psychodynamic psychotherapy . This method helps the patient recover a sense of self and learn new coping strategies and ways to deal with intense emotions related to the trauma. Typically, it consists of three phases:1) establishing a sense of safety for the patient; 2) exploring the trauma itself in depth; 3) helping the patient re-establish connections with family, friends, the wider society, and other sources of meaning.
- Discussion groups or peer-counseling groups. These groups are usually formed for survivors of specific traumas, such as combat, rape/incest, and natural disasters. They help patients to recognize that other survivors of the shared experience have had the same emotions and reacted to the trauma in similar ways. They appear to be especially beneficial for patients with guilt issues about their behavior during the trauma (such as submitting to rape to save one's life, or surviving the event when others did not).
- Family therapy . This form of treatment is recommended for PTSD patients whose family life has been affected by the PTSD symptoms.
Medications
In general, medications are used most often in patients with severe PTSD to treat the intrusive symptoms of the disorder as well as feelings of anxiety and depression. These drugs are usually given as one part of a treatment plan that includes psychotherapy or group therapy . As of 2002, there is no single medication that appears to be a "magic bullet" for PTSD. The selective serotonin reuptake inhibitors (SSRIs) appear to help the core symptoms when given in higher doses for five to eight weeks, while the tricyclic antidepressants (TCAs) or the monoamine oxidase inhibitors (MAOIs) are most useful in treating anxiety and depression.
Alternative therapies
Some alternative therapies for PTSD include:
- Spiritual/religious counseling. Because traumatic experiences often affect patients' spiritual views and beliefs, counseling with a trusted religious or spiritual advisor may be part of a treatment plan. A growing number of pastoral counselors in the major Christian and Jewish bodies have advanced credentials in trauma therapy.
- Yoga and various forms of bodywork are often recommended as ways of releasing physical tension or muscle soreness caused by anxiety or hypervigilance.
- Martial arts training can be helpful in restoring the patient's sense of personal effectiveness and safety. Some martial arts programs, such as Model Mugging, are designed especially for survivors of rape and other violent crimes.
- Art therapy, journaling, dance therapy, and creative writing groups offer safe outlets for the strong emotions that follow traumatic experiences.
Recent controversial therapies
Since the mid-1980s, several controversial methods of treatment for PTSD have been introduced. Some have been developed by mainstream medical researchers while others are derived from various forms of alternative medicine. They include:
- Eye Movement Desensitization and Reprocessing. This is a technique in which the patient reimagines the trauma while focusing visually on movements of the therapist's finger. It is claimed that the movements of the patient's eyes reprogram the brain and allow emotional healing.
- Tapas Acupressure Technique (TAT). TAT was derived from traditional Chinese medicine (TCM), and its practitioners maintain that a large number of acupuncture meridians enter the brain at certain points on the face, especially around the eyes. Pressure on these points is thought to release traumatic stress.
- Thought Field Therapy. This therapy combines the acupuncture meridians of TCM with analysis of the patient's voice over the telephone. The therapist then provides an individualized treatment for the patient.
- Traumatic Incident Reduction. This is a technique in which the patient treats the trauma like a videotape and "runs through" it repeatedly with the therapist until all negative emotions have been discharged.
- Emotional Freedom Techniques (EFT). EFT is similar to TAT in that it uses the body's acupuncture meridians, but it emphasizes the body's entire "energy field" rather than just the face.
- Counting Technique. Developed by a physician, this treatment consists of a preparation phase, a counting phase in which the therapist counts from 1 to 100 while the patient reimagines the trauma, and a review phase. Like Traumatic Incident Reduction, it is intended to reduce the patient's hyperarousal.
Prognosis
Trauma survivors who receive critical incident stress debriefing as soon as possible after the event have the best prognosis for full recovery. For patients who develop full-blown PTSD, a combination of peer-group meetings and individual psychotherapy are often effective. Treatment may require several years, however, and the patient is likely to experience relapses.
There are no studies of untreated PTSD, but long-term studies of patients with delayed-reaction PTSD or delayed diagnosis of the disorder indicate that treatment of patients in these groups is much more difficult and complicated.
In some patients, PTSD becomes a chronic mental disorder that can persist for decades, or the remainder of the patient's life. Patients with chronic PTSD often have a cyclical history of symptom remissions and relapses. This group has the poorest prognosis for recovery; some patients do not respond to any of the currently available treatments for PTSD.
Prevention
Some forms of trauma, such as natural disasters and accidents, can never be completely eliminated from human life. Traumas caused by human intention would require major social changes to reduce their frequency and severity, but given the increasing prevalence of PTSD around the world, these long-term changes are worth the effort. In the short term, educating people—particularly those in the helping professions—about the signs of critical incident stress may prevent some cases of exposure to trauma from developing into full-blown PTSD.
See also Anxiety reduction techniques ; Bodywork therapies ; Creative therapies ; Exposure treatment ; Somatization and Somatoform disorders
Resources
BOOKS
American Psychiatric Association. Diagnostic and Statistical Manual of Mental Disorders. 4th edition, text revised. Washington, DC: American Psychiatric Association,2000.
Beers, Mark H., M.D., and Robert Berkow, M.D., eds. "Posttraumatic Stress Disorder." In The Merck Manual of Diagnosis and Therapy, 17th edition. Whitehouse Station, NJ: Merck Research Laboratories, 1999.
Herman, Judith, M.D. Trauma and Recovery. 2nd ed., revised. New York: Basic Books, 1997.
Laub, Dori, M.D. "An Event Without A Witness: Truth, Testimony and Survival." In Testimony: Crises of Witnessing in Literature, Psychoanalysis, and History, written by Dori Laub, M.D. and Shoshana Felman. New York: Routledge, 1992.
ORGANIZATIONS
American Psychiatric Association. 1400 K Street NW, Washington D.C. 20005. <http://www.psych.org> .
Anxiety Disorders Association of America, Inc. 11900 Parklawn Drive, Suite 100, Rockville, MD 20852. (301) 231-9350. <http://www.adaa.org> .
International Critical Incident Stress Foundation, Inc. 10176 Baltimore National Pike, Unit 201, Ellicott City, MD21042. (410) 750-9600. Emergency: (410) 313-2473. <http://www.icisf.org> .
International Society for Traumatic Stress Studies. 60 Revere Drive, Suite 500, Northbrook, IL 60062. (847) 480-9028. <http://www.istss.org> .
National Center for PTSD. 1116D V.A. Medical Center, 215 N. Main Street, White River Junction, VT 05009-0001.(802) 296-5132. <http://www.ncptsd.org> .
National Institute of Mental Health. 6001 Executive Boulevard, Rm. 8184, MSC 9663, Bethesda, MD 20892-9663. (301) 443-4513. <http://www.nimh.nih.gov> .
Rebecca J. Frey, Ph.D.